The microbial community found in buildings is primarily a reflection of the occupants, and in the case of hospitals, the microbiota may be sourced from patients, staff, or visitors. In addition to leaving microbiota behind, occupants may pick up microorganisms from building surfaces. Most of the time, this continuous exchange of microorganisms between a person and their surroundings is unremarkable and does not raise concerns. But in a hospital setting with immunocompromised patients, these microbial reservoirs may pose a risk. Window glass, sills, and the surfaces around windows are often forgotten during hospital disinfection protocols, and the microbial communities found there have not previously been examined.
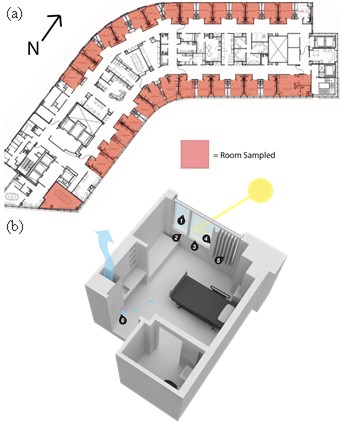
In a 2019 collaboration between the Biology and the Built Environment Center at the University of Oregon and the Oregon Health & Sciences University, we sampled various window surfaces from patient rooms in a hospital ward. We characterized the viable bacterial community located on these surfaces, and investigated the association of relative light exposure of the surface (in direct light or not), the cardinal direction of the room (and roughly the amount of total light exposure in a day), and proximity of the patient room to the nurses’ station (which has higher occupancy and traffic).
This paper is the first first-authored research paper from a former undergraduate mentee of mine at the University of Oregon; Patrick Horve.
Horve, P.F., Dietz, L., Ishaq, S.L., Kline, J., Fretz, M., Van Den Wymelenberg, K. 2020. Viable bacterial communities on hospital window components in patient rooms. PeerJ 8: e9580.
Abstract
Previous studies demonstrate an exchange of bacteria between hospital room surfaces and patients, and a reduction in survival of microorganisms in dust inside buildings from sunlight exposure. While the transmission of microorganisms between humans and their local environment is a continuous exchange which generally does not raise cause for alarm, in a hospital setting with immunocompromised patients, these building-source microbial reservoirs may pose a risk. Window glass is often neglected during hospital disinfection protocols, and the microbial communities found there have not previously been examined. This pilot study examined whether living bacterial communities, and specifically the pathogens Methicillin-resistant Staphylococcus aureus (MRSA) and Clostridioides difficile (C. difficile), were present on window components of exterior-facing windows inside patient rooms, and whether relative light exposure (direct or indirect) was associated with changes in bacterial communities on those hospital surfaces. Environmental samples were collected from 30 patient rooms from a single ward at Oregon Health & Science University (OHSU) in Portland, Oregon, USA. Sampling locations within each room included the window glass surface, both sides of the window curtain, two surfaces of the window frame, and the air return grille. Viable bacterial abundances were quantified using qPCR, and community composition was assessed using Illumina MiSeq sequencing of the 16S rRNA gene V3/V4 region. Viable bacteria occupied all sampled locations but was not associated with a specific hospital surface or relative sunlight exposure. Bacterial communities were similar between window glass and the rest of the room, but had significantly lower Shannon Diversity, theorized to be related to low nutrient density and resistance to bacterial attachment of glass compared to other surface materials. Rooms with windows that were facing west demonstrated a higher abundance of viable bacteria than those facing other directions, potentially because at the time of sampling (morning) west-facing rooms had not yet been exposed to sunlight that day. Viable C. difficile was not detected and viable MRSA was detected at very low abundance. Bacterial abundance was negatively correlated with distance from the central staff area containing the break room and nursing station. In the present study, it can be assumed that there is more human traffic in the center of the ward, and is likely responsible for the observed gradient of total abundance in rooms along the ward, as healthcare staff both deposit more bacteria during activities and affect microbial transit indoors. Overall, hospital window components possess similar microbial communities to other previously identified room locations known to act as reservoirs for microbial agents of hospital-associated infections.
Featured Image Credit: catinsyrup, iStock


