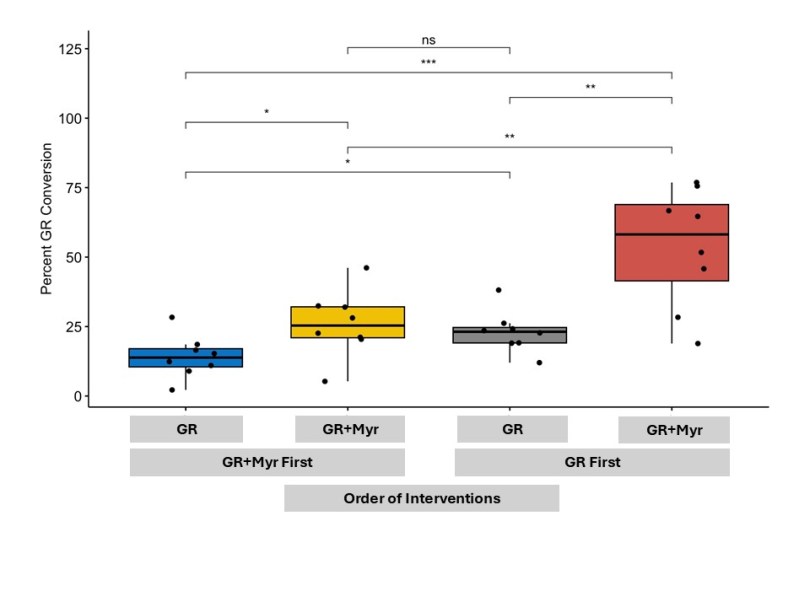
This study was run back in 2021 at Appalachian State University by Dr. Giuseppe Valacchi, Alessandra Pecorelli, and colleagues, when participants were given one dose of a glucoraphanin supplement combined with the plant enzyme myrosinase (which converts the GLR into the anti-inflammatory sulforaphane by the time the supplement gets to your small intestines), or one dose of the glucoraphanin supplement alone (in the absence of the plant enzyme, this requires gut microbes to convert GLR to SFN).
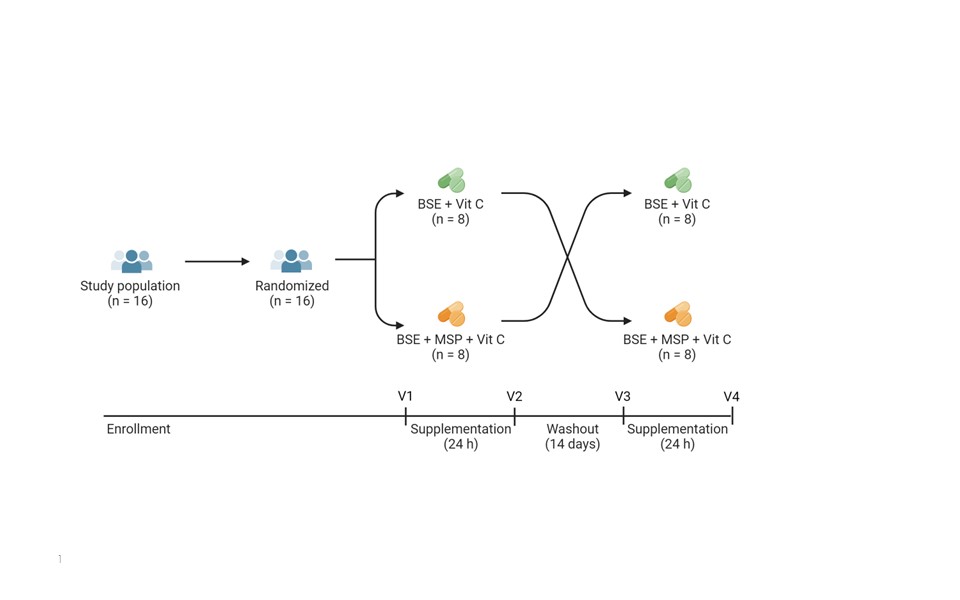

Since the Ishaq Lab is interested in how gut microbes can produce anti-inflammatories from inactive compounds in broccoli sprouts, and the Li Lab has been researching the use of sulforaphane for disease prevention and treatment for almost 20 years, Yanyan and I were a natural fit for this collaboration.
Yanyan and I were introduced to Dr. Jed Fahey when he joined the UMaine Institute of Medicine faculty network in 2022. We talked to Jed about his recent work Brassica Protection Products, a company he founded back in 1997 with Dr. Paul Talalay, and Yanyan and I were invited as collaborators in 2023 by Antony Talalay, CEO and Co-Founder, and Paul’s son.
As part of their dissertations, Marissa Kinney performed qPCR to quantify microbial genes during her master’s, and Lola Holcomb performed 16S rRNA bacterial community sequencing during her PhD. While Jed, Tony, and the BPP team are, of course, interested in how their supplement can be used to improve health, the Ishaq Lab is also interested in teasing apart why some people’s gut microbiome is very responsive to GLR supplementation and will produce a fair amount of sulforaphane, while other’s people’s gut won’t react to glucoraphanin at all.
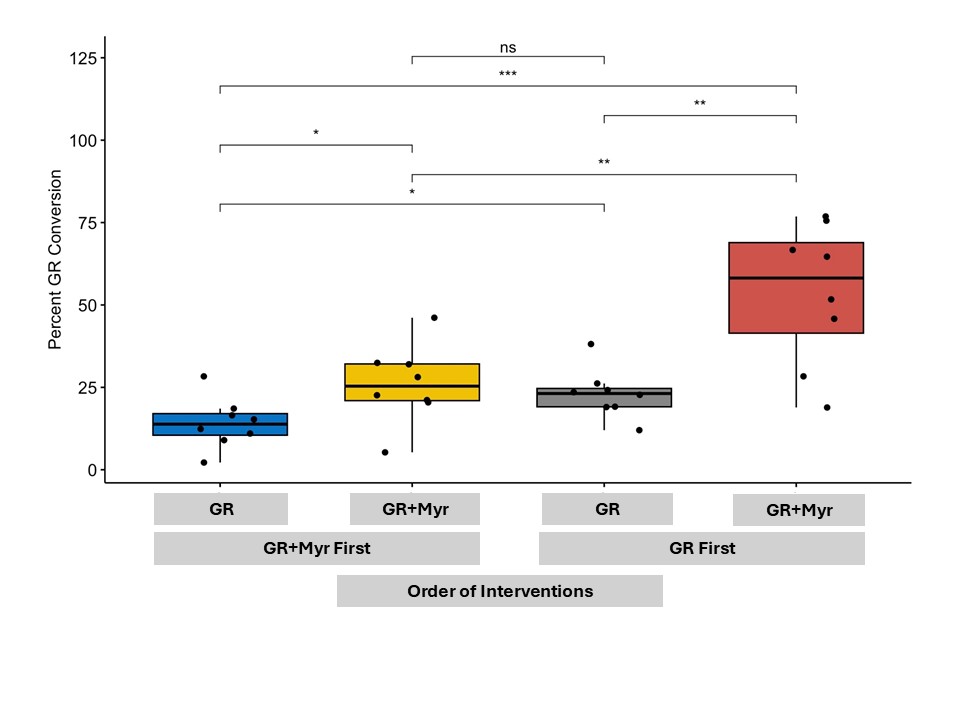
Even more intriguing were the participants in the study who had very little glucoraphanin conversion even when the myrosinase enzyme that can do the conversion was provided in the supplement. In fact, there was a lot of variability in how effective the enzyme was depending on the person- implying there are other biological or environmental factors at play which may be impeding the conversion of glucoraphanin into an anti-inflammatory.
Exogenous myrosinase from mustard seed increases bioavailability of sulforaphane from a glucoraphanin-rich broccoli seed extract in a randomized clinical study.
Angela Mastaloudis, Lola Holcomb, Jed W. Fahey, Camila Olson, David C. Nieman, Colin Kay, Robert O’Donnell, Alessandra Pecorelli, Marissa Kinney, Yanyan Li, Suzanne L. Ishaq & Giuseppe Valacchi. Scientific Reports, In Press. (2026)
Abstract: Inactive glucoraphanin (GR) in broccoli is converted to the antioxidant, anti-inflammatory, and anti-bacterial sulforaphane (SF) by cruciferous vegetable enzyme myrosinase (Myr), or similar enzymes from specific gut bacteria; both sources have variable efficiency. The effects of exogenous Myr on the conversion efficiency of GR to SF was compared to gut microbial Myr-like activity. In a randomized, double-blind, crossover study, sixteen subjects (9 F: 7 M) received a single oral dose of GR in broccoli seed extract with Myr-containing mustard seed powder, or broccoli seed extract alone, both with ascorbic acid. GR + Myr, on average, doubled the bioavailability of SF (39.8 ± 3.1%) compared to GR alone (18.6 ± 3.1%), and increased the conversion rate in the first 8 h (25.4% ± 2.7%) compared to GR alone (8.0% ± 2.7) based on measurement of urinary metabolites. There were no differences in fecal bacterial communities after the single dose; however, four bacterial GR-converting genes significantly correlated with GR conversion (p < 0.0155). To our knowledge, this is the first human study to simultaneously investigate (1) a well-defined Myr source, (2) broccoli seeds as source of GR, (3) prediction of gut microbial responsiveness to GR.